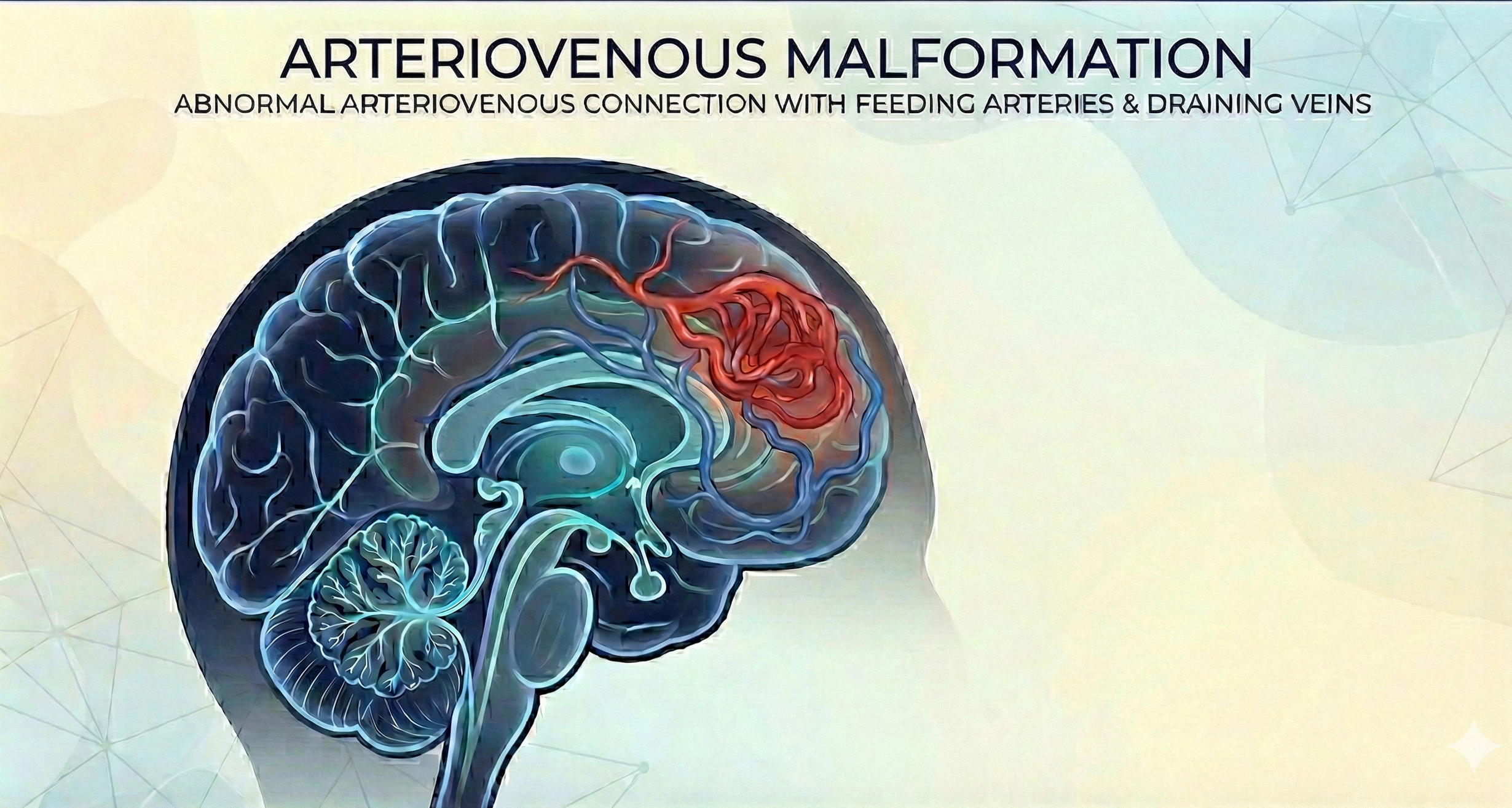
Brain Arteriovenous Malformation
An abnormal tangle of arteries and veins with altered blood flow. Treatment decisions involve carefully balancing the natural history risk against the risk of intervention — and radiosurgery offers a non-incisional path for selected patients.
Abnormal vascular tangle
A brain AVM is an abnormal connection between arteries and veins. It can present with hemorrhage, seizures, headaches, or be found incidentally.
Multiple treatment options
Microsurgery, endovascular embolization, and stereotactic radiosurgery — often chosen based on AVM size, location, and risk profile.
Radiosurgery works gradually
AVM obliteration can take years after radiosurgery. Hemorrhage risk may persist until closure is confirmed on imaging.
What is a brain AVM?
A brain arteriovenous malformation (AVM) is an abnormal tangle of blood vessels where arteries connect directly to veins without the usual network of tiny capillaries in between. This creates a high-flow shunt that can weaken vessel walls and increase the risk of bleeding into the brain.
Brain AVMs vary widely in size, location, and hemorrhage risk. Some are found incidentally on imaging done for other reasons, while others present with hemorrhage, seizures, or headaches. The "right" treatment plan depends on individualized risk balancing.
Individualized risk balancing
Every AVM treatment decision involves weighing the natural history risk (what happens if the AVM is left alone) against the risk of treatment. Not every AVM needs to be treated — and when treatment is appropriate, the best approach depends on your AVM's specific characteristics.
Who may be a candidate for Gamma Knife radiosurgery?
Radiosurgery is most often considered when:
Candidacy is determined by a multidisciplinary team evaluating your AVM's size, location, and overall risk profile.
-
✓The AVM is relatively small or in a location where open surgery carries higher neurologic risk.
-
✓A multidisciplinary team determines radiosurgery offers a favorable risk/benefit profile compared with other strategies (surgery, embolization, or observation).
Gamma Knife Radiosurgery for AVMs
Radiosurgery offers a non-incisional approach to AVM obliteration — but it's important to understand that the effect is gradual and unfolds over years, not days.
How Gamma Knife Works for AVMs
Focused radiation is delivered to the AVM nidus, triggering changes in the vessel walls that lead to gradual thickening and eventual closure of the abnormal vessels.
Understanding the Delayed Nature of Radiosurgery for AVMs
Unlike radiosurgery for tumors — where the goal is to stop growth — AVM radiosurgery aims for complete vessel closure (obliteration). This biological process takes time, typically years. During this period, the AVM may still carry a risk of hemorrhage. Your team will counsel you on what this means for your specific situation and follow-up plan.
What to Expect
The treatment day itself is outpatient — but the biological effect unfolds over years, making long-term follow-up essential.
Before
MRI and angiographic imaging for precise targeting. Counseling on the delayed nature of benefit — including the important fact that hemorrhage risk persists until the AVM is fully obliterated.
During
Stereotactic immobilization is placed, followed by DSA angiography for real-time vascular mapping, treatment planning, and radiation delivery. The procedure is non-incisional and completed within a single day.
After
Follow-up imaging over time to assess the AVM's response and confirm obliteration. This typically involves periodic MRI and eventually repeat angiography. Additional treatments may be considered if residual AVM remains.
Benefits and Risks
Potential Benefits
- Non-incisional path to AVM obliteration in selected patients
- Outpatient treatment with quick recovery from the procedure itself
- Can treat AVMs in deep or eloquent locations where surgery carries higher risk
- Avoids the immediate surgical risks of craniotomy
Possible Risks
- Continued hemorrhage risk — the AVM can still bleed until fully obliterated, which may take years
- Delayed radiation effects — swelling, neurologic changes that may develop months after treatment
- Seizures — can occur as a presenting symptom or after treatment
- Incomplete obliteration — some AVMs may require additional treatment
Patient FAQs
If radiosurgery is outpatient, why is follow-up so long?
Can an AVM still bleed after radiosurgery?
When to Seek Urgent Care
Call 911 or go to the ER immediately for sudden severe headache, seizure, new weakness or numbness, trouble speaking, or sudden vision changes.